Tech Support: Technological Infrastructure for Psychedelic Therapy
An update of recent developments
One of the most intriguing angles to explore the emerging psychedelic landscape is the concurrent adoption of digital health technology1.
A year ago, in atai’s Enabling Technologies; Trends in Digital Health & Neurotech: Part 1, I posited:
The timing of the psychedelic emergence is auspicious as three coinciding paradigm shifts are also underway and can be thought of as the “Set and Setting” for the nascent field of psychedelic science and medicine:
The ‘Neuroplastic Revolution2’
Adoption and development of Digital Health Technologies
The Personalized Medicine Movement
For a time, psychedelics x technology was the sole focus of my writing, and while I am now returning to cover the broader playing field, it remains a key theme and area of interest.
A few recent developments make it timely to revisit this area:
Group VR experiences can produce ego attenuation and connectedness comparable to psychedelics
Homecoming Releases Comprehensive Preparation Program for Ketamine Therapy Providers
Disclosure: Beckley Waves is an investor in Homecoming and of course has shared founders with Beckley Psytech. I have also consulted with the Homecoming team.
I want to take a stab at positioning these recent developments within the trends mentioned earlier to view them within the larger context of this emerging field.
But before we jump into today’s dispatch…
A few weeks ago, I had the honor of sharing the stage with Rachel Yehuda, the director of the Center for Psychedelic Psychotherapy and Trauma Research at Mt. Sinai, and Matias Serebrinsky, Partner at Psymed Ventures at the Soho House in New York. Our conversation is captured in the latest episode of the Business Trip Podcast. We cover a wide range of topics, including:
The promise and the hype of psychedelics as therapeutics
The challenges of psychedelic research
The future of research and clinical practice
The broad array of policy approaches
Take a listen!
Digital Psychedelics: A Maturing Virtual Reality?
Virtual Reality (VR) strikes me as both incredibly promising and entirely underwhelming. I couldn’t be more disappointed with my Oculus Quest II experience.
Perhaps that is because I was moved to make the purchase based on this excerpt from VRx: How Virtual Therapeutics Will Revolutionize Medicine:
“I vacate my body and watch it as my consciousness drifts up toward the ceiling. I sense a brief existential crisis, a sort of Cartesian fit where my mind and body seek to reconcile the separation. For the first time in my life, I am disconnected from myself. I cannot tell if this is a physical or metaphysical cleavage, but it doesn’t really matter. It feels as if I have been extracted from my body. I am floating like a balloon. Now I am up in the ceiling looking down upon my lifeless self… I’ve become an ethereal and disembodied entity hovering above my shell of a body below. That body down there is not moving. My arms are moving—I can feel them—but that body is not. I am in motion but that body is still. That body is unresponsive.”
Sounds wild, right? Sign me up.
Except, none of the available programs or games I have tried come remotely close to this.
Last week I spoke with David Glowacki, a VR researcher and co-founder of VR start-up aNUma, about his recent study titled Group VR experiences can produce ego attenuation and connectedness comparable to psychedelics.
I told him about my disappointment with the current state of VR, and he assured me the future is on its way.
The reason for my disappointment, he suggested, is that many of the VR programs on the market today are trying to deliver common experiences—like meetings, concerts, video games, and sporting events—through VR.
He believes VR will start to get interesting with high-quality experiences that are ONLY possible through VR.
And this is what his recent paper is pointing to.
The specific VR program, Isness—licensed for commercialization by aNUma—demonstrated comparable effects to moderate to high doses of psychedelics as measured by validated scales commonly used in psychedelic research.
From the abstract (emphasis added):
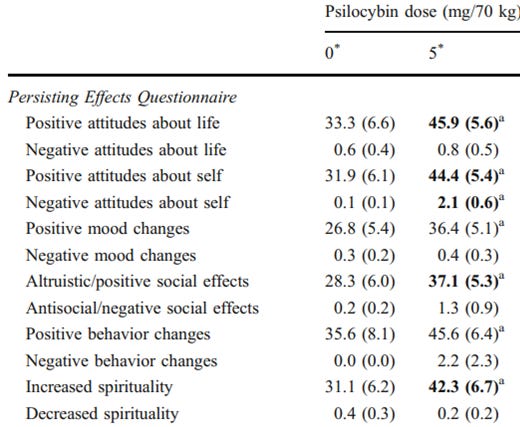
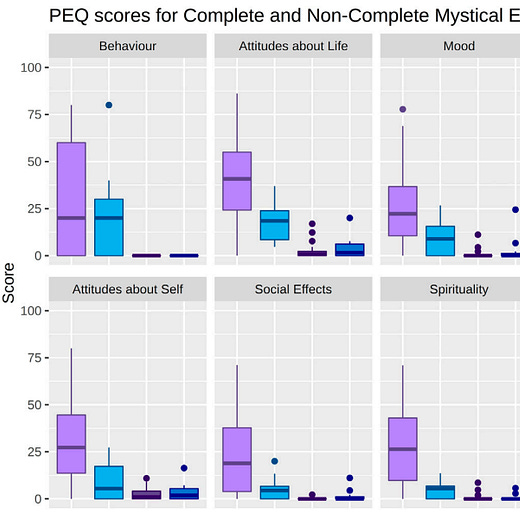
“We analyzed the results (N = 58) using 4 different self-report scales previously applied to analyze subjective [Psychedelic Drug] phenomenology (the inclusion of community in self scale, ego-dissolution inventory, communitas scale, and the MEQ30 mystical experience questionnaire). Despite the complexities associated with a distributed experiment like this, the Isness-D scores on all 4 scales were statistically indistinguishable from recently published [Psychedelic Drug] studies, demonstrating that distributed VR can be used to design intersubjective [Self Transcendant Experiences] where people dissolve their sense of self in the connection to others.
Isness is a group VR experience in which several participants engage at the same time but in different parts of the world—an example of “decentralized” or “distributed” research—an approach that strikes me as particularly useful to consider for psychedelic research, especially for naturalistic/real-world study designs.
Most interesting to me is, what the authors call energetic coalescence, “a new class of embodied intersubjective experience where bodies can fluidly merge, enabling participants to include multiple others within their self-representation.”
This is an example of an experience only possible in Virtual Reality.
Glowacki told me:
“… there is cool stuff going on in VR, but it’s not the stuff that’s so readily available. And for me, it’s really important to highlight the good stuff, so Mel Slater is someone that I like to highlight because he’s done a lot of very interesting stuff where you leave your body, and then you re-inhabit your body or you swap perspectives with other people. That is stuff that I think is interesting, because you can’t do that stuff in any way in this conventional four dimensions that we inhabit normally. So for me, it’s really interesting because there’s a reason to use VR in these cases that’s really compelling.”
I sense that the VR projects that have identified the psychedelic space as the grounds for commercial application and adoption, such as aNUma, Enosis Therapeutics, and Entheo Digital, will have been inspired by psychedelics and thus create experiences that, as Glowacki describes, are only possible in VR.
In other words, hopefully, we will see psychedelics and this flavor of VR as the primary examples of ‘Experiential Medicine’—interventions that leverage experience-dependent neuroplasticity to drive psychological and neurobiological change.
Beckley PsyTech x Empatica
A few weeks ago, Beckley Psytech announced a partnership that fits all three trends noted above: the adoption of digital health tech (wearables) and the move towards personalized medicine.
From the press release:
Beckley Psytech Limited, a private company dedicated to addressing neurological and psychiatric disorders through the novel application of psychedelic medicines, and Empatica, Inc., a medical wearables and digital biomarker company offering continuous, passive, and unobtrusive monitoring for patients with neurological conditions, today announced that the companies have entered into a partnership to support the collection and analysis of behavioural and physiological data in Beckley Psytech’s future clinical trials…
“This partnership will utilise Empatica’s medical-grade EmbracePlus wearable and software, to identify and measure passive behavioural and physiological signals in the upcoming Phase 2 studies evaluating the use of 5-MeO-DMT in combination with psychotherapy in the treatment of treatment resistant depression (TRD).”
This is a good opportunity to revisit the concept of Digital Phenotyping and Digital Biomarkers.
I had previously written about digital biomarkers’ role as outcome measures in clinical trials in place of validated surveys and questionnaires or as tools to define disease states.
For example, in Psychedelics & Digital Phenotyping, I suggested:
Digital Phenotyping promises that it will solve the problem of quantifying subjective conditions that have no objective markers—the kind of conditions that psychedelic medicine is most interested in treating.
Depression, PTSD, Addiction have no viral loads; there are no confirmatory blood tests; there is no objective diagnosis.
But I don’t think this was entirely right. Rather than replacing validated outcome measures or redefining psychiatric nosology, there is a much more practical use case for digital biomarkers: predicting responders before treatment and relapse before it occurs.
But this also points to potential drug-software combination products, again from atai's Enabling Technologies; Trends in Digital Health & Neurotech: Part 1:
Drug-software Combination Products are gaining in popularity.
The cardinal example of a drug-software combination product is Pear Therapeutics’ Reset-O which combines a prescription smartphone app that provides cognitive behavioral therapy, fluency training, and contingency management, with the prescription drug buprenorphine, for the treatment of Opioid Use Disorder (OUD).
The thinking is that many treatments, such as buprenorphine for OUD, could be improved with a “tech layer” that is low risk and synergistic, thus improving treatment adherence and/or efficacy.
Fascinating times at the intersection of psychedelics and technology.
Homecoming Unveils KAP Preparation Platform
Again for disclosure, Beckley Waves is an investor in Homecoming, and I have done some consulting with the team.
I once worked with a therapist who “prescribed” The Feeling Good Handbook, a workbook companion to our therapy sessions.
The publisher describes it as “Filled with charts, quizzes, weekly self-assessment tests, and a daily mood log, The Feeling Good Handbook actively engages its readers in their own recovery.”
It complemented our therapy work and provided educational content and the format for active engagement in my therapeutic process. Also, the completed exercises, journal entries, and quizzes became a record of my work which I have had the chance to reflect on occasionally.
I think of Homecoming as developing a digital version of this process for Psychedelic Assisted Therapy with an emphasis on preparation and support.
Recently Homecoming announced a program for Ketamine Assisted Psychotherapy preparation:
“Homecoming’s ketamine-assisted therapy (KAP) platform was created in partnership with experienced ketamine providers to offer thorough educational content about how to prepare for a ketamine therapy experience. This includes the stages of therapy, talking to your friends and family about psychedelic therapy, ketamine and music, activities, lessons, and reflections to support patients’ journeys. In addition, clinicians utilizing Homecoming have the opportunity to choose from a variety of supplemental tools and assessments that support the processing of insights gained during ketamine therapy experiences.”
This is a critical program because ketamine clinics are on the rise, and there are at least three challenges for the emerging field of ketamine-assisted therapy:
Training sufficient numbers of therapists for KAP/PAT
Reimbursement for KAP
Patient education and support
Educational and support content will be essential features for the thousands of people turning to ketamine for the first time.
Furthermore, the punctuated nature of KAP and PAT are radical departures from the relatively constant or gradual conventional 50-minute once-a-week therapy format.
Education, preparation, and integration around periodic/occasional psychedelic treatments is an added layer of complexity for therapists, and this is where a product like Homecoming’s preparation program fits in.
Patients working with ketamine for the first time will have many questions, and if education and support material can be delivered in conjunction with their therapist, rather than unreliable information online, it can help make for successful treatment.
Further Developments
BusinessInsider: Psychedelics aren't going to upend mental healthcare anytime soon. Here's how long it will be until the emerging field turns research into reality.
“But drug development is a time-consuming and expensive process, and there are no guarantees that any of the companies in the industry will navigate it successfully. Despite the excitement around the medical potential of psychedelics, even the industry leaders are years away from getting any medical treatment approved by US regulators, according to an Insider analysis. Plus, the companies are almost certain to need millions, if not billions, more in cash to fund their work.”
Hopkins’ Effect Size Higher than European Counterparts
That’s it for this week, thanks for reading!
Zach
For further treatment of this topic, see the following:
In the same ‘atai’ piece, I put forward the following idea regarding the adoption of neuroplastic techniques:
However, harnessing the power of neuroplasticity for the precise, targeted stimulation of specific brain regions or networks —Applied Neuroplasticity— is in its infancy.
Neuroplasticity has been relegated to an explanation, not a practice.
This seems about to change with the advent of
Psychedelics and Psychoplastogens
Neuromodulation techniques like Neurofeedback, Virtual Reality, Transcranial Direct Current Stimulation, and Closed-Loop Experiential Medicine
The idea that the brain and nervous system are malleable seems to have reached an inflection point. Neuroplasticity as a popular culture idea stems back to Norman Doidge’s The Brain that Changes Itself.
Around the same time, this was published, a feature in Time Magazine by the late science writer Sharon Begley also sounded the alarm about the scientific revolution at hand:
“FOR DECADES, THE PREVAILING DOGMA IN neuroscience was that the adult human brain is essentially immutable, hardwired, fixed in form and function, so that by the time we reach adulthood we are pretty much stuck with what we have… this view held that if genes and development dictate that one cluster of neurons will process signals from the eye and another cluster will move the fingers of the right hand, then they'll do that and nothing else until the day you die…But research in the past few years has overthrown the dogma. In its place has come the realization that the adult brain retains impressive powers of "neuroplasticity"--the ability to change its structure and function in response to experience.